Healthcare Data Fundamentals explains how health information is captured, cleaned, standardized, stored, and prepared for analysis. It covers data types, sources, governance, integration, and technical skills, helping professionals ensure quality, privacy, and usability for reporting, analytics, and AI applications.
Every day, hospitals, labs, insurers, and digital health platforms generate massive amounts of clinical and operational data. From electronic records to imaging outputs and pharmacy transactions, modern healthcare runs on information.
Yet organizations struggle to find professionals who can manage it. Errors in coding, privacy, or interpretation can delay treatments, compromise research, trigger compliance risks, or cost millions. Employers increasingly seek people who can capture, standardize, validate, secure, and prepare healthcare data for analysis.
For newcomers, the systems are complex, regulations strict, and accuracy non-negotiable. Learning healthcare data fundamentals turns confusion into clarity, helping you understand:
- Where data originates
- How it moves between systems
- What quality checks are required
- How privacy and compliance are maintained
- How datasets are prepared for analytics and AI
These skills open doors to roles in clinical data management, health informatics, medical coding, analytics support, and AI-enabled healthcare operations. This guide walks you through the essential knowledge blocks, from data types and sources to cleaning, governance, and preparation for advanced technologies, giving you the foundation to thrive in modern healthcare careers.
What is Healthcare Data Fundamentals?
Healthcare data fundamentals refer to the essential understanding of how health information is generated, organized, protected, and applied across care settings. This knowledge helps professionals work accurately with clinical and technical teams, maintain data quality and privacy, and prepare information for reporting, analytics, and AI applications.
What Healthcare Data Fundamentals Covers?
Healthcare data fundamentals give professionals the skills to handle information accurately and confidently. Key areas include:
- Understand Major Data Categories:
Professionals learn to manage various types of healthcare data, including clinical data (diagnoses, treatments, lab results), operational data (scheduling, staffing), financial data (billing, claims, reimbursements), public health data (surveillance, outcomes), and patient-generated data (wearables, apps, surveys).
- Capture Data Accurately:
Professionals are taught how to accurately capture data using Electronic Health Records (EHRs), voice-based documentation, or automatic inputs from medical devices and wearables. This also includes ensuring standardized formats and real-time capture, and converting free-text notes into standardized codes (e.g., ICD, SNOMED).
- Track Information Flow:
This involves understanding how data moves across healthcare systems (EHRs, labs, pharmacies), ensuring integration and seamless linkage across systems, and maintaining audit trails for compliance and reporting accuracy.
- Apply Standards and Formats:
Professionals learn to apply healthcare standards such as ICD, SNOMED, LOINC, and CPT to ensure data consistency and interoperability. They also focus on the use of data formats like HL7 and FHIR for standardized data exchange.
- Ensure Data Quality and Governance:
This area covers ensuring data completeness and consistency through validation, quality control processes, and regular auditing. It also includes implementing governance protocols to maintain accountability, transparency, and regulatory compliance.
- Protect Privacy and Ethics:
Focuses on handling sensitive data in compliance with regulations such as HIPAA and GDPR, with an emphasis on implementing access controls, data encryption, and obtaining informed consent for ethical use of data.
- Manage the Data Lifecycle:
Professionals learn how to manage healthcare data from creation and secure storage to access and archival, ensuring data retention in line with legal and regulatory standards.
- Prepare Reporting and Analytics:
This area prepares professionals to transform raw data into actionable insights by generating operational and financial reports, creating predictive models, and preparing AI-ready data for decision-making, diagnosis support, and clinical decision systems. Data visualization tools are also covered for creating dashboards that support healthcare administration.
These competencies enable professionals to support informed decisions, reporting, and AI applications in healthcare.
Types and Sources of Healthcare Data
Types
Healthcare information is divided into categories because each type serves a different purpose in delivering and managing care.
| Types | What is it? |
|---|---|
| Clinical Data | Information related to patient diagnosis, treatment, and medical history used to guide care delivery. |
| Operational / Administrative Data | Data that supports scheduling, staffing, workflows, and the overall management of services. |
| Financial Data | Monetary information such as billing, claims, reimbursements, and expenses used for financial planning. |
| Patient-Generated Data | Health details reported directly by individuals, often through apps or monitoring devices. |
Sources
Healthcare data is collected from multiple sources because each area of healthcare generates information for a specific purpose. Categorization makes it easier to record, retrieve, protect, and apply data accurately.
| Sources | What are they? |
|---|---|
| Electronic Health Record (EHR) | Digital records of patient care that support treatment decisions, operations, compliance, and analytics. |
| Laboratory and Diagnostic Systems | Generate test and imaging results that inform diagnosis, therapy, and monitoring. |
| Administrative and Billing Systems | Capture registrations, encounters, claims, and payments to manage workflows and finances. |
| Pharmacy Systems | Document prescriptions, dispensing, and inventory to ensure medication safety and control. |
| Clinical Research Systems | Manage study data, participant information, and documentation for trial oversight and evaluation. |
| Patient- and Device-Generated Sources | Collect health inputs from individuals via wearables and remote tools to support continuous care. |
Healthcare Data Foundations: How Healthcare Data Is Captured, Structured, and Stored
Healthcare information is gathered during patient care, diagnostics, administration, and research through digital systems designed to ensure accuracy and traceability. Once recorded, it is organized into defined formats so it can be searched, shared, and analyzed efficiently.
Behind the scenes, databases manage day-to-day transactions, while larger repositories consolidate historical data from multiple departments. Together, these structures make information reliable, secure, and ready for reporting, analytics, and AI applications.
1. Data Capture in Clinical Settings
Healthcare data is captured through multiple channels to ensure accuracy, reliability, and completeness:
- Clinician and Nurse Entry at the Point of Care: Direct input during consultations, procedures, and rounds using electronic health records.
- Voice-Based Documentation and Dictation: Provider notes are spoken and transcribed into the system.
- Automatic Capture from Medical Devices: Vital signs, lab results, imaging outputs, and wearables feed data directly.
- Conversion of Notes into Standardized Codes: Narrative notes are translated into structured codes for reporting and analysis.
- Information Submitted by Patients: Data collected through forms, portals, surveys, or remote monitoring.
- Research and Trial Data Collection: Study-specific information entered via controlled electronic forms.
- Upload of External Documents and Images: Reports, referrals, and scans are imported and indexed.
These capture methods form the foundation for all downstream processes, including validation, governance, and analytics.
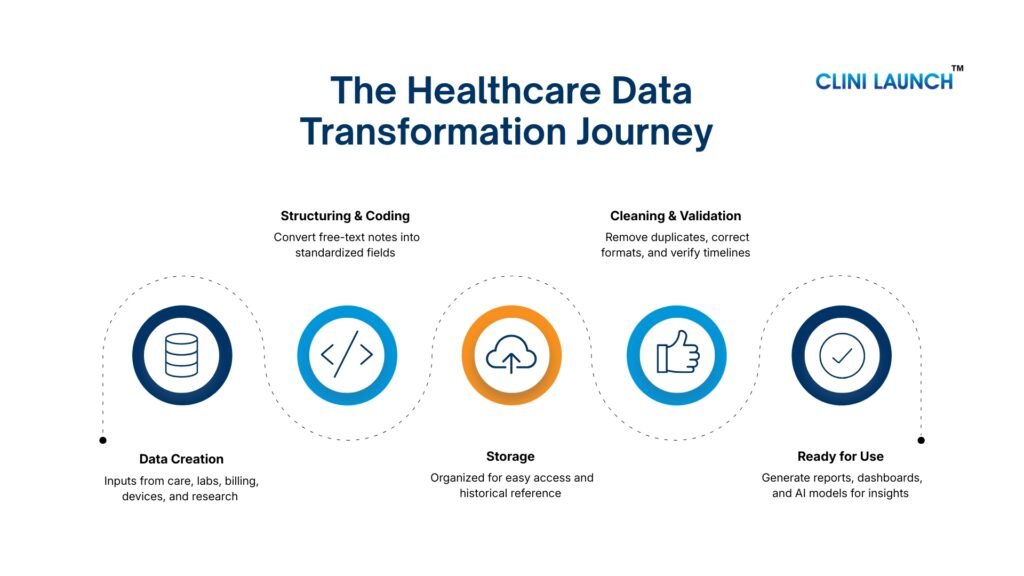
2. How Unstructured Data is converted into Structured Healthcare Data
Much healthcare information exists in free-text formats, such as doctor notes, discharge summaries, or imaging reports. While these contain valuable clinical insights, they cannot be easily analyzed, reported, or used for AI in their raw form. Converting unstructured data into structured formats ensures that:
- Extraction of Key Element: Text from notes, discharge summaries, imaging reports, or patient messages is scanned to identify meaningful elements such as symptoms, diagnoses, procedures, or medications.
- Natural Language Processing (NLP) / AI Tools: Algorithms parse the text, recognize entities, and assign them to predefined categories. For example, “shortness of breath” is flagged as a symptom.
- Human Verification / Review: Specialists check and correct automated outputs to ensure accuracy, especially for ambiguous or context-dependent information.
- Structuring in Databases: Verified information is stored in structured fields within EHRs, clinical databases, or research systems, ready for querying, reporting, or analysis.
- Integration with Existing Structured Data: Newly structured data is linked to patient records, lab results, or other datasets to create a complete, longitudinal view.
3. Standard Coding Systems (ICD, SNOMED, LOINC, CPT)
Standard coding systems are a core part of healthcare data fundamentals because they ensure that clinical information is structured, consistent, and ready for analysis. They play a critical role in each stage of the data lifecycle:
- Capture: Codes like ICD-10, SNOMED CT, LOINC, and CPT are applied during data entry or abstraction to convert narrative notes, lab results, and procedure details into standardized formats.
- Structuring: These codes transform raw, free-text information into discrete, analyzable fields within electronic health records, research databases, and clinical repositories.
- Storage: Coded data is stored in relational databases, data warehouses, or linked repositories, enabling consistent retrieval and integration across systems.
- Analysis and Reporting: Structured, coded data allows for reliable querying, aggregation, dashboards, regulatory reporting, and AI/ML applications.
4. Databases, Data Warehouses, and Cloud Storage in Healthcare
Modern healthcare relies on multiple storage layers to keep information organized, accessible, and secure. Data from clinical systems, labs, imaging units, and administrative platforms is continuously generated and managed using different technologies tailored to specific needs.
- Databases for Day-to-Day Operations:
- Relational databases capture patient visits, lab results, prescriptions, and scheduling details.
- Designed for fast entry, retrieval, and updates, these systems allow care teams to access accurate information in real time.
- Data Warehouses for Consolidation and Analysis:
- Information from multiple databases is gathered, cleaned, and standardized within a data warehouse.
- By preserving historical data and ensuring consistency, warehouses support reporting, trend analysis, research, and AI-driven analytics.
- Cloud Storage for Scalability and Collaboration:
- Cloud platforms offer scalable storage to accommodate the growing volume of healthcare data.
- They also provide collaborative access and high-performance computing resources for advanced analyses.
5. Regulatory and Security Frameworks Governing Data
Healthcare data contains personal and sensitive information. Protecting it isn’t just legal, it’s essential for patient trust and safe care. Here’s how organizations keep it secure while still using it for treatment, research, and innovation:
- Access Control: Only authorized roles like doctors, nurses, and analysts can view or modify relevant information.
- Identity Verification: Secure logins and multi-factor authentication confirm every user’s identity.
- Encryption: Data is protected both in storage and while moving across networks.
- Audit Trails: Every access, edit, or transfer is logged and monitored for unusual activity.
- Policies and Training: Staff follow clear rules for collection, storage, sharing, and retention.
- Anonymization: Personal identifiers are removed when data is used for research or AI.
- Compliance Checks: Continuous oversight ensures adherence to legal and ethical standards.
By combining these safeguards, healthcare organizations maintain secure, trustworthy data that drive decisions, research, and AI innovation all while preserving patient privacy.
AI&ML in Healthcare
Step into the future of healthcare by mastering AI and ML applications. Learn to work with clinical data, create predictive models, and drive smarter decisions in patient care, operations, and research.

Duration: 12 months
Skills you’ll build:
Other Courses
How Healthcare Data is prepared for Analysis
Before any dashboard, prediction, or AI model can be trusted, healthcare data must be prepared carefully. Real-world medical information is rarely ready for immediate use. It comes from multiple systems, in different formats, with gaps, duplicates, and inconsistencies.
Because of this, professionals working in analytics, clinical research, or AI often spend a major portion of their time transforming raw information into reliable, structured, and interpretable datasets.
1. Data Cleaning and Preprocessing in Healthcare
Data cleaning and preprocessing is the process of checking and fixing data so it can be trusted and used for decisions, research, or AI. Key steps include:
- Finding duplicates: Spotting repeated patient records or test results.
- Checking missing information: Flagging missing details and deciding if they need to be added or clarified.
- Fixing formats: Correcting mistakes like wrong dates or numbers in the wrong place.
- Spotting unusual values: Identifying results that don’t make sense, like extremely high or low lab values.
- Checking for logic errors: Making sure data makes sense, e.g., discharge dates come after admission dates.
- Fixing simple errors: Correcting clear mistakes when it’s easy to know what’s right.
- Flagging complex problems: Marking unclear or tricky issues for experts to review.
- Keeping track of changes: Recording what was corrected so everything is transparent.
- Making sure the data is ready: Checking that the dataset is clean enough for reports, research, or AI.
2. Data Normalization and Standardization
Healthcare data comes from multiple departments, devices, and professionals, so measurements, labels, and formats often vary. Normalization and standardization ensure this information is consistent and usable for analysis.
How it works:
- Convert units and formats: Align measurements (e.g., centimeters → meters) and unify date formats.
- Unify labels: Standardize categories like gender, test types, or procedure names.
- Map values to a common scale: Ensure scores, ranges, or ratings are comparable across sources.
- Check for consistency: Identify and correct values that don’t match expected rules or patterns.
- Prepare data for analysis: Once standardized, data can be aggregated, compared, and used in reports or AI models.
3. Handling Clinical Terminology Variability
Medical language varies the same condition can be documented in multiple ways, e.g., “heart attack,” “myocardial infarction,” or abbreviations. To make this data usable, it must be standardized.
Who does it:
- Clinical data specialists or health informatics teams review records and ensure terms are consistent.
- Automated tools assist with large datasets.
How it is done:
- Mapping terms: Different ways of saying the same thing are linked to a single standardized concept.
- Automated extraction: Tools like NLP identify key clinical concepts from free text.
- Verification: Experts check that automated mappings are correct.
4. Data Integration Across Multiple Systems
A patient’s records are often spread across hospitals, laboratories, pharmacies, and insurance providers, with each system storing information separately. To get a complete and accurate view, this data must be combined and harmonized.
How it happens:
- Matching and linking records: Patient identifiers, visit dates, and other key information are used to ensure records from different systems belong to the same individual.
- Resolving conflicts: Teams handle overlapping timelines, duplicate entries, or contradictory information.
- Standardizing formats: Units, labels, and terminology are aligned before merging datasets.
- Validating data: Checks are performed to ensure completeness and correctness.
- Creating a unified dataset: Cleaned and standardized records are consolidated into a single dataset ready for reporting, research, or analytics.
Tools & Platforms Used in Healthcare Data Fundamentals
| Workflow Step | Common Tools | Purpose |
|---|---|---|
| Data Cleaning & Preprocessing | SQL, Python, SAS, IBM data platforms | Remove duplicates, fix missing values, correct formats, detect inconsistencies |
| Normalization & Standardization | SQL, Python, SAS, ETL tools (Talend, Informatica, Microsoft SSIS), healthcare platforms (Epic, Cerner) | Align units, standardize labels, unify terminology across datasets |
| Terminology Standardization | SNOMED CT, ICD-10, LOINC, NLP tools, coding platforms | Map free-text clinical notes to standard concepts for consistency and analytics |
| Data Integration | ETL tools, SQL, Python/R, Epic/Cerner integration modules, data quality dashboards | Merge records from multiple systems, resolve conflicts, and create a unified dataset |
| Data Storage | Relational databases, data warehouses, cloud storage (AWS, Azure) | Store structured and processed data securely, maintain historical records, enable analytics |
| Data Analysis & AI Preparation | SAS, Python, R, analytics dashboards | Aggregate, query, visualize, and prepare datasets for reporting, research, and AI/ML models |
Key Challenges in Using Healthcare Data for AI and ML
Artificial intelligence and machine learning can support diagnosis, prediction, and operational planning. However, their performance is directly tied to how healthcare data is collected, organized, and controlled. When information is incomplete, inconsistent, or poorly governed, even advanced models struggle to produce dependable results. The following challenges commonly affect the practical use of healthcare data in AI and ML initiatives.
1. Data Fragmentation Across Healthcare Systems
Healthcare information is often distributed across multiple providers and databases that function independently. Because patient histories are not consolidated, AI and ML models are trained on partial or inconsistent datasets. This limits pattern discovery, weakens predictive performance, and complicates longitudinal modelling.
2. Interoperability and Standardization Barriers
The health data interoperability market was valued at about USD 84.6 billion in 2025 and is expected to grow to over USD 350 billion by 2032 (CAGR ≈ 22.6 %). This reflects huge demand for harmonizing data across systems.
AI systems require large, well-structured, and comparable datasets. However, variations in software platforms, terminologies, and documentation formats make data exchange difficult. Significant preprocessing, mapping, and normalization are needed before algorithms can be trained, increasing time, cost, and technical complexity.
3. Bias and Imbalanced Clinical Data
Machine learning outcomes are shaped by the data used for training. When certain populations are underrepresented, variables are missing, or labels carry human subjectivity; models may deliver skewed predictions. These distortions can reduce generalizability and create uneven performance across patient groups.
4. Privacy and Ethical Concerns in AI Models
AI development depends on access to detailed personal information, which raises concerns about confidentiality, consent, and responsible reuse. In addition, opaque decision pathways in complex models make it difficult to explain outcomes, creating ethical challenges around accountability and fairness.
5. Regulatory Constraints in AI Deployment
Before algorithms can be integrated into care settings, they must demonstrate safety, transparency, and clinical validity. Regulatory expectations demand rigorous testing and documentation, which can slow innovation but are necessary to ensure trustworthy AI adoption.
How Machine Learning Uses Healthcare Data
Machine learning enables computers to study medical information and use what they learn to make informed predictions. Rather than following fixed instructions, these systems continuously improve as they are exposed to more data.
They can examine elements such as laboratory findings, diagnoses, medications, and patient records. In addition, they are capable of learning from medical images and written clinical documentation.
Why Strong Data Foundations Are Critical for AI
The global AI in healthcare market was valued at around USD 36.7 billion in 2025 and is projected to reach over USD 500 billion by 2033, growing at nearly a 39 % annual rate, driven by demand for predictive analytics, diagnostics, and decision support.
AI models learn directly from historical healthcare information. If records contain gaps, duplicate entries, inconsistent coding, or outdated values, the system may learn the wrong lessons and produce misleading predictions.
For example, a risk model cannot correctly identify deterioration if vital signs are recorded at irregular intervals. Imaging algorithms cannot perform well if labels differ between departments. Predictive tools struggle when patient histories are split across disconnected systems.
Reliable AI therefore requires structured capture, standardized terminology, consistent updates, and clear data lineage. Teams must know where information originated, how it was modified, and whether it is complete.
When these foundations are in place, models become more accurate, easier to validate, and safer to introduce into clinical environments.
Management (iHealth) Training
The PG Diploma in Intelligent Healthcare Management bridges traditional healthcare with AI, analytics, and automation. It equips professionals to optimize operations, drive innovation, and lead in digital healthcare through practical skills in data-driven decision-making, workflow optimization, and ethical governance.

Duration:12 months
Skills you’ll build:
Other Courses
Core Technical Concepts in Healthcare Data Foundations
Building a career in healthcare analytics or AI happens in stages. Moving straight into advanced modeling without first understanding how clinical data is captured, arranged, and supervised often creates knowledge gaps.
A stepwise approach helps aspirants strengthen their foundation, gain professional credibility, and develop skills that match real workplace expectations.
The sequence below reflects how many industry-oriented training pathways prepare future professionals.
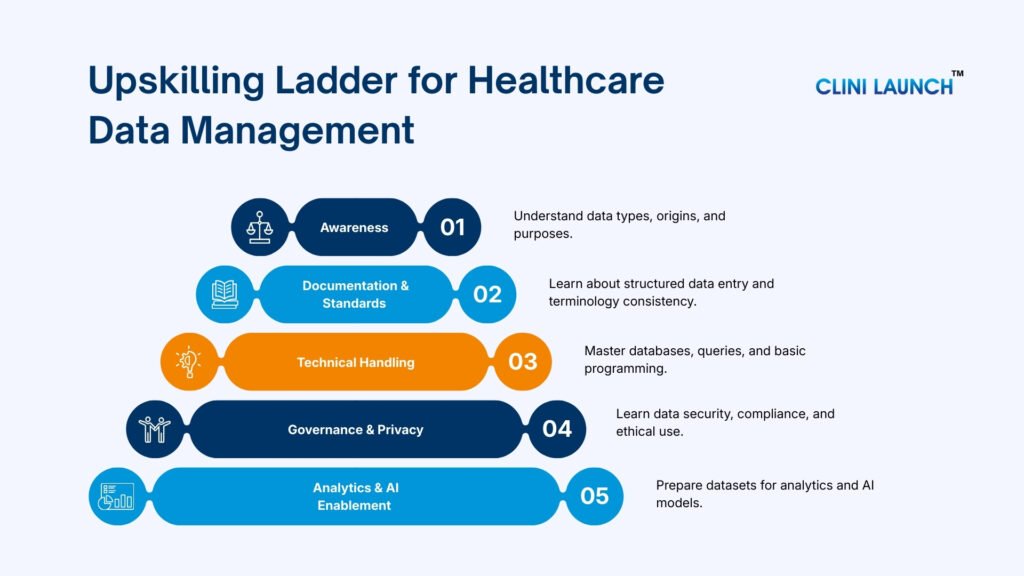
1.Understanding Healthcare Databases and SQL Concepts
The first milestone is understanding how healthcare information is maintained inside digital systems. Hospitals and research organizations rely on databases where data is stored in structured formats across related tables. Becoming familiar with this environment is essential before attempting analysis.
Focus areas
- How tables, rows, and fields are organized
- The role of patient identifiers and links
- Writing simple SQL queries
- Producing basic data extracts
Outcome
- Confidence in retrieving the right data for reporting, checks, or analysis.
2 . Basics of Statistical Thinking in Healthcare
After learning to access information, the next responsibility is understanding what it represents. Statistical reasoning supports accurate interpretation and helps avoid misleading conclusions.
Focus areas
- Common measures like averages and variation
- Spotting trends over time
- Difference between relationships and causes
- Understanding probability and risk
Outcome
- Ability to explain whether findings are significant and useful.
3. Fundamentals of Data Modeling
As knowledge grows, aspirants should learn how real clinical processes are converted into system designs. Proper structure ensures that analytics remain consistent and reliable.
Focus areas
- Relationships among patients, visits, tests, and treatments
- Why uniform standards are necessary
- How structure influences accuracy
Outcome
- Better coordination with technology and analytics teams.
4. Basics of Programming in Healthcare Analytics (Python/R Overview)
At this level, professionals begin to manipulate data directly rather than depend on others. Basic programming expands the ability to prepare and explore information at scale.
Focus areas
- Preparing and cleaning raw inputs
- Automating repeated activities
- Creating simple charts
- Formatting data for further modeling
Outcome
- Greater efficiency and readiness for advanced analytical work.
5. Introduction to Healthcare Data Governance
Handling healthcare information requires awareness of responsibility. Understanding governance principles ensures safe, ethical, and lawful data use.
Focus areas
- Who can access information
- Recording and monitoring changes
- Responsible handling
- Awareness of regulatory expectations
Outcome
- Professional credibility and suitability for real-world environments.
Conclusion
Healthcare is becoming deeply data-driven. From routine documentation to advanced prediction systems, every improvement in quality, safety, and efficiency depends on how well information is captured, standardized, protected, and interpreted.
Understanding these fundamentals is what separates surface knowledge from true employability. When professionals know where data originates, how systems connect, why governance matters, and how preparation influences analytics, they can confidently participate in reporting, research, automation, and AI initiatives.
Strong foundations turn complex environments into manageable workflows. They allow you to communicate with clinicians, collaborate with IT teams, and contribute to decisions that directly affect outcomes.
If building these capabilities is your goal, structured guidance can accelerate the journey.
At CliniLaunch, the learning pathway is designed to move step by step, from databases and standards to analytics, compliance, and real-world healthcare applications. The focus remains on practical exposure, industry expectations, and readiness for modern roles.
Explore the programs, understand the roadmap, and begin building expertise that healthcare organizations actively look for.
FAQs – Healthcare Data Fundamentals
1. What are Healthcare Data Fundamentals?
They are the core principles of how health information is captured, organized, standardized, stored, and prepared for analysis, reporting, and AI applications.
2. Why is understanding healthcare data important?
Proper handling of healthcare data ensures accurate patient care, reliable research, compliance with regulations, and successful AI and analytics initiatives.
3. What types of healthcare data exist?
Clinical data, operational/administrative data, financial data, and patient-generated data, each serving different decision-making purposes.
4 . Where does healthcare data come from?
Data is collected from electronic health records (EHRs), labs, imaging systems, pharmacy records, administrative platforms, clinical research systems, and patient-generated sources.
5 . How is unstructured data converted into structured data?
Through extraction of key elements, natural language processing (NLP) or AI tools, human verification, database structuring, and integration with existing records.
6 . What role do standard coding systems play?
ICD, SNOMED, LOINC, and CPT codes standardize clinical information for interoperability, accurate reporting, and analytics.
7 . How is healthcare data stored and managed?
Through relational databases for daily operations, data warehouses for consolidated historical data, and cloud platforms for scalable storage and collaboration.
8 . How is healthcare data prepared for analysis?
It involves cleaning, preprocessing, normalization, standardization, and integration to ensure it is accurate, consistent, and ready for reporting or AI use.
9 . What are the key challenges with healthcare data for AI and ML?
Data fragmentation, interoperability barriers, bias, imbalanced datasets, and privacy or ethical concerns can impact AI model performance.
10 . How does strong data management improve AI outcomes?
Reliable, structured, and standardized data enables accurate predictive modeling, better decision support, and safer deployment of AI in healthcare.